Article • Cloud Computing
Virtual fracture clinic boosts patient care
A fracture clinic model being pioneered by a UK hospital is improving patient care and delivering significant cost savings for the NHS
Mark Nicholls
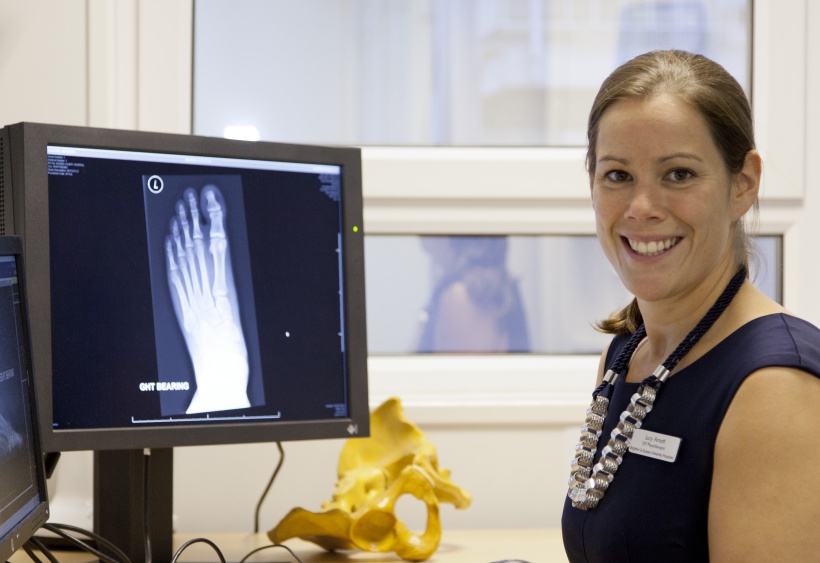
The Virtual Fracture Clinic (VFC) established by the Brighton and Sussex University Hospitals NHS Trust sees patients with broken bones or soft tissue injury supported through video links and self-management methods, rather than make additional journeys to hospital for face-to-face appointments with orthopaedic consultants.
The trust says the initiative also makes better use of consultant time by allowing specialists to focus more on their own areas of expertise. The clinic was originally set up after orthopaedic consultant James Gibb became concerned that the existing model of care – where patients attending emergency departments with fractures were assessed and then booked in for a further appointment with an on-call orthopaedic consultant - was inefficient.
However, that meant they did not necessarily see the best person for their specific injury – a spinal specialist may be seeing someone with a broken toe, for example. ‘It was a bit of a lottery,’ said Lucy Cassidy, the trust’s VFC project lead. ‘Now, when a patient attends A&E, instead of being put on a list to see someone face to face, they are referred for a virtual consultation.
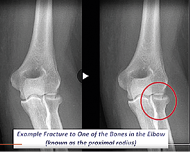
‘This consultation involves an orthopaedic consultant looking through each case, and depending on the type of injury, the patient is placed on a self-management pathway and supported with rehab videos online. Or if they had an injury that needed to be seen, they would be booked into an appointment with the right specialist and receive the appropriate management.’ Patients have access to a rehab adviser within 72 hours of their injury, saving them having to come in to hospital with a generic fracture clinic consultant before being referred on.
The model is based on a virtual clinic in Glasgow, but has been taken a significant step further in Brighton by adding the physiotherapy component. ‘Our service is now more streamlined and we find a large percentage of our patients can be self-managed, where they do not even need to come in for an appointment, ‘ Cassidy added. ‘We decided to design with a physiotherapy-led service because we found patients were not being given much information to self-manage injuries.’
The VFC has 27 rehab videos hosted on YouTube, presenting patients with six weeks’ worth of rehab across various injuries. Giving patients the correct information at the outset of their treatment journey is helping to reduce long-term problems.
Brighton has 4,500 adult general fracture clinic cases and 3,000 wrist and hand injury patients a year with plans to expand to paediatric cases next year. With the virtual appointment half the price of a £150 (170 euro) face-to-face appointment, there are significant cost savings for the NHS from the project, for which Microsoft supplies software and part-funds the initiative. ‘It also means that our hospital consultants can be redeployed to maximise their skills,’ Cassidy pointed out.
Within the trust, this has meant additional ward rounds for neck or femur fracture patients, while other hospitals have held additional clinics or helped increase theatre capacity. ‘We are basically using the workforce to maximise their skills set rather than using them in a generic fracture clinic way.’

While there are clear staff resource benefits, putting figures on internal savings is more difficult, but it does mean less imaging, fewer registrars using clinics, reception staff time saved, and patient journeys down with carbon footprint reduced. Current figures show that 57% of patients referred to the VFCs are discharged or placed on SOS appointments - where they are on self-management but can regain contact for support - after first referral from A&E, compared to a previous discharge rate of approximately 40% in the traditional model.
The initiative has reduced outpatient appointments by 57%, saving the NHS more than £750,000 (€850,000), with 2,000 fewer patients having to visit the hospital a year. Mrs Cassidy said patient satisfaction is up and, since January, the hospital has been collecting data to help manage referrals and ultimately to measure outcomes by coding every injury, to enable clinicians to look at the functional outcome for each injury and assess patient progress.
Profile
Lucy Cassidy is an advanced practice physiotherapist and leader of the Brighton and Sussex NHS Trust’s Virtual Fracture Clinic project.
03.11.2017