Prostate Cancer
Fusion targeted biopsy proves more accurate in diagnosis
New research confirms that an innovative procedure combining MRI and ultrasound to create a 3D image of the prostate can more accurately locate suspicious areas and help diagnose whether it’s prostate cancer.
Using specialized equipment needed, physicians at UT Southwestern Medical Center’s Harold C. Simmons Comprehensive Cancer Center began using the fusion biopsy procedure about three years ago for its ability to blend live ultrasound images with captured MRI images. The fused image creates the 3D model, and flags anomalies that could be areas of concern. That helps guide urologists to get tissue samples called biopsies to determine whether cancer is present.
UT Southwestern’s early adoption of the cutting-edge technology allowed researchers to report on the superior diagnostic performance of this novel approach compared to traditional methods for diagnosing prostate cancer. Furthermore, these researchers have partnered with colleagues in Brazil to conduct follow up studies that now show the technique consistently improved detection of clinically significant prostate cancer under a wide variety of conditions, even when radiologists were using different equipment and protocols.
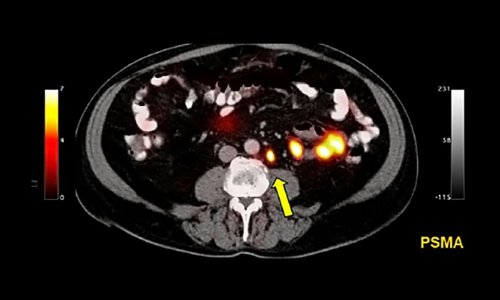
“In the past, we diagnosed prostate cancer by random biopsies of the prostate in men with elevated PSA values. With fusion biopsy, we actually find more cancer, we can differentiate between dangerous tumors and less aggressive tumors, and in some cases we perform fewer biopsies,” said Dr. Daniel Costa, Assistant Professor of Radiology and with the Advanced Imaging Research Center (AIRC) at UT Southwestern.
Prostate cancer is the second most common cancer diagnosed in men, after skin cancer. Prostate cancer risk increases with age, with most cases occurring after age 60. According to the National Cancer Institute (NCI), about 180,890 men will be diagnosed this year, and about 14 percent of men will be diagnosed sometime during their lifetime.
The procedure, technically known as MRI-TRUS (magnetic resonance imaging/transrectal ultrasound) fusion targeted prostate biopsy, requires special imaging capabilities and high level training for both radiologists and urologists, so its use has not become widespread.
It works like this: after the urologist identifies a patient at risk for prostate cancer, radiologists use a state-of-the-art MRI examination to identify potentially suspicious areas. If present, the MRI images are then sent to a device that blends those with an ultrasound used by urologists to take a biopsy or sample of the tissue in question to determine whether it has cancer.
“In many instances, MRI-TRUS biopsies performed at UT Southwestern have allowed us to diagnose and treat aggressive prostate cancer in patients whose prior biopsies failed to find the cancer,” said Dr. Ivan Pedrosa, Chief of the Division of Magnetic Resonance Imaging, Associate Professor of Radiology and with the Advanced Imaging Research Center, who holds the Jack Reynolds, M.D. Chair in Radiology. “Because of its improved precision, patients and physicians are better informed to choose the most appropriate treatment. This helps to avoid surgery in patients with less aggressive disease, and ensures that patients with more aggressive cancers are identified earlier.”
The fusion biopsy technique has been used for nearly 1,000 patients at UT Southwestern. “Patients diagnosed at a later stage of disease, or with a more aggressive cancer, have lower rates of survival, making it vital that we quickly identify those who are at the highest risk,” said Dr. Claus Roehrborn, Chair and Professor of Urology, who holds the E. E. Fogelson and Greer Garson Fogelson Distinguished Chair in Urology and the S.T. Harris Family Chair in Medical Science, in Honor of John D. McConnell, M.D. “The close collaboration between radiology and urology, and the ability to exchange the images and information across a common network, enhances the productivity of this collaboration and the outcomes for our patients.”
Prostate cancer forms in tissues of the prostate, a gland in the male reproductive system found below the bladder and in front of the rectum. The prostate surrounds the urethra, the tube through which urine flows. A healthy prostate is about the size of a walnut. If the prostate grows too large, it squeezes the urethra. This may cause difficulty in urinating, burning or pain during urination, more frequent urges to urinate at night, loss of bladder control, and blood in the urine. These symptoms may also have a different cause, so men with prostate symptoms should speak with their physician, Dr. Roehrborn said.
Source: UT Southwestern
26.09.2016