© Jo Panuwat D – stock.adobe.com
Article • Radiology workflow at RSNA 2025
Time-saving tactics for overburdened radiologists (without AI)
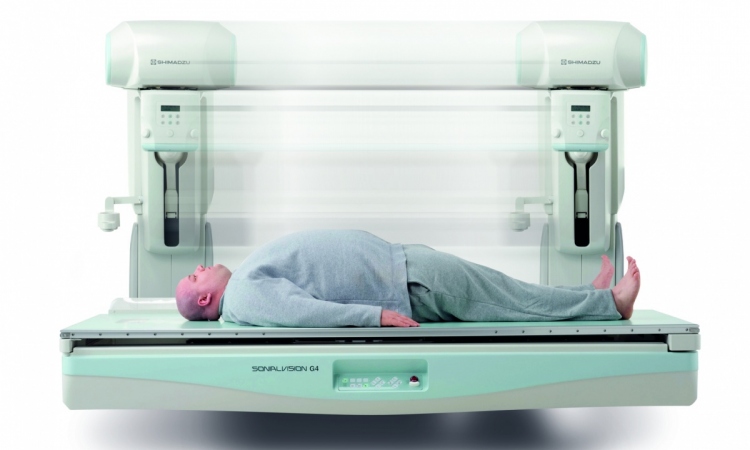
Radiologists worldwide are facing mounting workloads, with exam volumes rising and workforce numbers struggling to keep pace. At the RSNA 2025 annual meeting in Chicago, a dedicated session explored how departments can improve efficiency using tried-and-tested methods – without waiting for artificial intelligence to arrive.
By Cynthia E. Keen
Within this decade, AI is expected to become a landmark technology for radiology departments, having an impact on the way radiologists work comparable to the introduction of CT, MRI, and PET scanners or PACS. Its widespread deployment in future years will aid the fewer per-capita radiologists who will be interpreting a larger volume of exams than today – a higher percentage of which will be of advanced imaging complexity.
Radiologists today feel overburdened. What can be done now? The RSNA session, entitled 'Improving radiologist efficiency: what can you do while waiting for AI?', tackled this issue. It was a throwback session reminiscent of the 1990s, when radiology departments were trying to manage conversion from a film-based department to the first clunky and cumbersome generations of PACS. Radiologists faced greater inefficiencies while trying to adapt to a new efficiency-promoting technology. The recommendations in this session are as applicable as they were in the 1990s. It is just that two generations of radiologists may not think about them.
Identifying what wastes radiologists’ time
Inefficient department workflow is often a culprit, and classic rules to identify workflow inefficiency for any profession apply. From a quality control standpoint, so also are:
- Activities that do not add value
- Activities that add value but are not efficiency-optimised
- Tasks that could be automated
- Tasks that could be performed by a non-radiologist
James V. Rawson, MD, Vice Chair of Operations and Special Projects in Radiology at Beth Israel Deaconess Medical Center (BIDMC) in Boston, advises that his hospital's patient transfer policies had to be changed. Patients would not be admitted without the transferring hospital's CT images. With only a report, BIDMC had to repeat the exam, wasting both department scanning resources and radiologists' time.
How much time do you spend with new radiologists? Do you throw them into the reading room with an unfamiliar PACS? Or do you train them, and if so, how thoroughly?
James V. Rawson
Internally, when dictating either a low-value exam report or an addendum, it is important to ask why. Much has been published about reducing the orders of low-value exams, using clinical decision support software or directly communicating with the ordering physician. With respect to report addendums – what is causing the need to prepare this? Is it the arrival of comparisons after report dictation? If so, what can be done to prevent the situation from happening again?
Regularly evaluate data that can be automated, Dr Rawson advises. Auto-population of data and measurements is routine. Can other data measurements be added? Standardise as much as possible. He said that published studies have shown that standardised dictation macros of incidental findings management, for example, will be read more by ordering physicians. Departments should routinely determine if radiologists are performing tasks that others in the department could do. If so, optimise qualified staff to do these jobs.
Finally, Dr Rawson asked: 'How much time do you spend with new radiologists? Do you throw them into the reading room with an unfamiliar PACS? Or do you train them, and if so, how thoroughly?' An investment of one to three hours of familiarisation with a diagnostic workstation's software can pay huge dividends in an individual radiologist's workflow efficiency.
Standardization across a multi-hospital network
Developing best practice protocols for eight separate radiology practices serving 22 geographically dispersed hospitals with 18 to 510 beds is the way that the Canyons Region of Intermountain Healthcare, a health system servicing the entire state of Utah, efficiently operates. This is managed with a lot of education, communication, feedback, and constant review to maintain best practice protocols that standardise radiology services throughout the state.
We look to simplify processes, because that is how we gain efficiency
Marta E. Heilbrun
Marta E. Heilbrun, MD, Medical Director of Imaging Services, Quality and Patient Safety at Intermountain Healthcare, discussed how this uniformity happens for the hospitals and 143 clinics with 30,500 caregivers. 'We engage radiologist system leaders and their cross-group networks of section leaders to identify and maintain best practice protocols,' she said. 'We look to simplify processes, because that is how we gain efficiency.'
Rollout of new and updated protocols is done with attention to detail, and incorporates a mechanism for direct feedback from radiologists, managers, and technologists. 'We provide the entire network with supportive resources and a formal process to accomplish the work. We set and promote expectations by working with frontline technologists.'
All locales have the same scanners and utilise the same protocols. Documentation is standardised. Macros have been developed for every possible exam combination, to enable radiologists to incorporate standard recommendations into their reports. Workloads are consolidated several times in a 24-hour day, so that expertise is always available. Flexible scheduling is promoted for equitable work/life balance. Feedback and recommendations for improvement also have a schedule, with input from all involved carefully evaluated. Changes are made for the good of the entire network.
The workstation mouse: a help or a hindrance?
Mouse efficiency matters. In a single shift, a mouse travels 1.37 miles with 10,778 total input actions, Shawn Lyo, MD, a neuroradiologist at the University of Pennsylvania in Philadelphia, told RSNA attendees. ‘Choosing the right mouse and developing healthy usage habits can significantly enhance productivity and reduce strain. Eighty-seven percent of radiologists report musculoskeletal discomfort in a weekly basis,’ he said.
How to choose the right mouse? The decision is personal. Noting that shape impacts grip comfort, different shapes may work best for different sized hands. Weight is important, because lighter mice can improve speed. A heavier mouse can dampen unintended motions. Scrolling speed? Programmable buttons? ‘A mouse is a central component of a diagnostic workstation. How you optimize depends on your personal ergonomics, task demands, and computing environment. Optimising your mouse isn’t a luxury. It’s a practical investment in comfort, speed, and longevity,’ said Dr. Lyo.
Reducing radiologist’s interruptions
At one point, we recorded interruptions every three minutes
Alexander J. Towbin
Radiologists get interrupted. Daily interruptions may number in the hundreds in busy reading rooms of academic hospitals, caused by clinicians visiting the reading room to ask questions, by telephone calls, and by pagers, text messaging and urgent emails. ‘At one point, we recorded interruptions every three minutes,’ said Prof. Alexander J. Towbin, MD, a paediatric radiologist and Associate Chief Medical Information Officer at Cincinnati Children’s Hospital in Ohio.
Cincinnati Children’s radiology department was one of the first in the United States to create reading room assistant (RRA) positions. RRAs answer phone calls, answer general questions, communicate critical results, and engage with reading room visitors and ‘direct traffic’.
Radiologists enrol their professional private telephone numbers in a federal government registry to prevent scam and nuisance calls. Access to these telephone numbers by hospital staff is severely restricted, forcing callers to direct inquiries to RRA. Phone ‘trees” are redesigned and improved for callers as needed, so that they expeditiously direct a caller to the person they ultimately needed to talk to.
‘We also evaluated workflow. RRA desks were relocated to the entrance of each reading room. With visitors having immediate access to RRAs when they enter a reading room, reading rooms have become quieter and less disruptive from a visual perspective’. Stefanie Woodard, DO, a breast imager at the Heersink School of Medicine at the University of Alabama in Birmingham augmented Prof. Towbin’s remarks by discussing the essentials of optimal reading room design.
03.03.2026